Many of you know I have worked in an Infant Pulmonary Function Laboratory (IPFT) for nearly 30 years. This type of work isn’t done in many pediatric hospitals for a number of reasons, one of the most relevant being there is no commercially available equipment for many of the tests. That is why most of my work involves writing the computer software to do this type of testing, as well as putting the equipment/hardware together to perform the tests.
Almost ten years ago we developed a system to measure how well gases diffuse between the lung alveoli and the capillary blood supply that surrounds these air sacs. Oxygen diffuses out of the lungs into the blood, and the carbon dioxide produced by the body’s cells diffuses the other direction, from the blood into the air sacs, and then exhaled from the body. Ours is actually the only lab in the world able to do this test on babies.
To do this test, a system of valves first inflates the baby’s lungs with air for a couple of breaths to help them relaxed. They are mildly sedated and asleep during this. Then at the end of a breath, the valves switch to a test mixture containing Helium (He) and a small concentration of carbon monoxide (CO). Helium is an inert gas, and does not diffuse out of the alveoli. Thus the difference in the Helium concentration between what is inhaled and what is exhaled is determined by the amount of air in the lung. The more air, the more the He is diluted, and the greater the difference. This way, we can measure the volume of air in the infant’s lung.
CO on the other hand rapidly diffuses into the blood, so the difference between what is inhaled and exhaled represents how well gases diffuse.

The reason for this post at this time is that I’ve been putting together this new portable version of the system for these past couple of weeks. The box on the very bottom is the balloon valve controller, that inflates/deflates the balloons to deliver the right gas at the right time, and controls when inspiration and expiration occurs. The box with the mess of cables is the interface between the computer and the balloon valve controller and another electronic flow control valve, as well as reading the signals from the amplifiers and transducers measure airflow, volume, and pressures. (I’ll be cleaning that up now that the system is working).
This video shows the various balloons opening and closing during the test, inflating a test lung.
Here is the results screen of the software I’ve written.
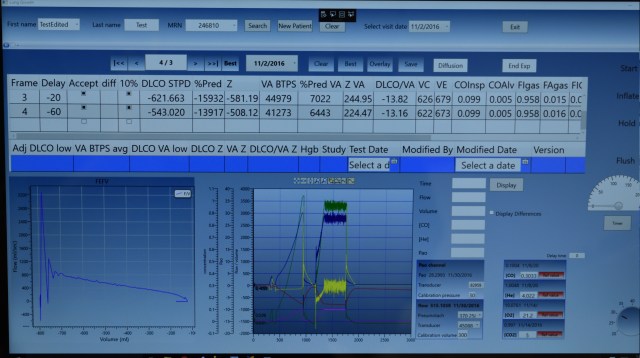
These are some publications from our lab using the lung diffusion system.
- Castillo Andres; Llapur Conrado J; Martinez Tanya; Kisling Jeff; Williams-Nkomo Tamica; Coates Cathy; Tepper Robert S. Measurement of single breath-hold carbon monoxide diffusing capacity in healthy infants and toddlers. Pediatric pulmonology 2006;41(6):544-50.
- Balinotti Juan E; Chakr Valentina C; Tiller Christina; Kimmel Risa; Coates Cathy; Kisling Jeffrey; Yu Zhangsheng; Nguyen James; Tepper Robert S Growth of lung parenchyma in infants and toddlers with chronic lung disease of infancy. American Journal of Respiratory and Critical Care Medicine 2010;181(10):1093-7. Department of Pediatrics, Indiana University Medical Center, James Whitcomb Riley Hospital for Children, 702 Barnhill Drive, Indianapolis, IN 46202-5225, USA.
- Valentina C. Chakr, MD, Conrado J. Llapur, MD, Edgar E. Sarria, MD, PhD, Rita Mattiello, PT, MS, Jeffrey Kisling, RRT, Christina Tiller, RRT, Risa Kimmel, RN, Brenda Poindexter, MD, and Robert S. Tepper, MD, PhD, Ventilation Homogeneity Improves with Growth Early in Life, Pediatr Pulmonol. 2012 Apr;47(4):373-80.
- Daniel V. Chang, Christina J. Tiller, Jeffrey A. Kisling, Jamie Case, Julie A. Mund, Laura S. Haneline, David A. Ingram and Robert S. Tepper, Membrane and capillary components of lung diffusion and pro-angiogenic cells in infants, Eur Respir J. 2014 Feb;43(2):497-504.
- Ehsan Z, Montgomery GS, Tiller C, Kisling J, Chang DV, Tepper RS., An infant with pulmonary interstitial glycogenosis: clinical improvement is associated with improvement in the pulmonary diffusion capacity. Pediatr Pulmonol. 2014 Mar;49(3):
- Assaf SJ, Chang DV, Tiller CJ, Kisling JA, Case J, Mund JA, Slaven JE, Yu Z, Ahlfeld SK, Poindexter B, Haneline LS, Ingram DA, Tepper RS., Lung parenchymal development in premature infants without bronchopulmonary dysplasia. Pediatr Pulmonol. 2015 Dec;50(12):1313-9
- Chang DV, Assaf SJ, Tiller CJ, Kisling JA, Tepper RS., Membrane and Capillary Components of Lung Diffusion in Infants with Bronchopulmonary Dysplasia. Am J Respir Crit Care Med. 2016 Apr 1;193(7):767-71
